Keloids are raised, and scar tissue growth develops due to exaggerated skin healing after trauma. These unsightly scars cross the boundaries of the original injury and often grow progressively more prominent over time. Patients with dark skin tones and family history seem predisposed to developing keloids, especially in highly mobile areas prone to tension like the chest or shoulders.
While a variety of invasive treatments to flatten or remove mature keloids exist, the consensus remains that prevention is the cornerstone for avoiding these challenging scars. So, if prone to keloids, How Do I Prevent Keloid Scars from ever forming in the first place?
This article outlines evidence-based strategies both patients and practitioners can utilise before, during and after procedures to promote routine wound healing instead of exuberant fibrosis characteristic of keloids. From gentle tissue handling to anti-inflammatory drugs, choosing the proper prophylactic techniques for your situation may make all the difference for optimal, scar-free recovery.
How do I prevent keloid scars? Use silicone gel sheets.
Silicone gel sheets create an occlusive layer over a healing wound, which provides hydration and prevents excessive collagen production.
Dubai Keloid Management is a special healthcare service in dubai that helps people get rid of keloid scars, which are raised areas of skin caused by an overgrowth of scar tissue.
Book A Consultation With Dr Shehzadi Tasneem
Top-rated Plastic Surgeon For Keloid in Dubai
Installment Plan Available
- Apply silicone sheets for 12+ hours daily for about 12 months
- Use sheets after surgery on areas prone to keloids
- Studies show sheets reduce hypertrophic and keloid scarring
- Occlusion limits fibroblast activity and collagen synthesis
- Must have high patient adherence for effectiveness
- Provides a non-invasive option for prophylaxis
Gentle handling of wounds prevents keloids.

Handling wound beds during procedures preserves tissue viability and prevents additional inflammation.
- Limit tension when suturing wounds
- Minimise tissue trauma from instruments
- Prevent contamination and infection
- Consider non-invasive or less invasive options
- Do not overtly manipulate healing wounds
- Evert wound edges when closing excisions
Keloid prevention after surgery.
There are several evidence-based steps surgeons can take preoperatively to minimise the risk of postoperative keloid formation.
- Avoid making incisions in high-tension areas.
- Close wounds with minimal tension using deep sutures
- Inject the site with steroids at the time of closure
- Apply silicone gel sheets after the sutures are removed
- Consider radiation for high-risk wounds
- Schedule intralesional steroid injections PRN
- Educate the patient to minimise trauma to the site
Avoid wound tension to prevent keloids.
Excessive tension across a healing wound has been associated with an increased risk of pathologic scarring.
- Select low-tension wound closure techniques
- Distribute tension across the entire closure
- Close dead space to prevent fluid accumulation
- Immobilise the site to limit mechanical forces
- Reinforce the wound with adhesive strips
- Consider secondary revision if needed
- Educate patients on wound care restrictions
Steroid injections prevent keloids from getting more significant.
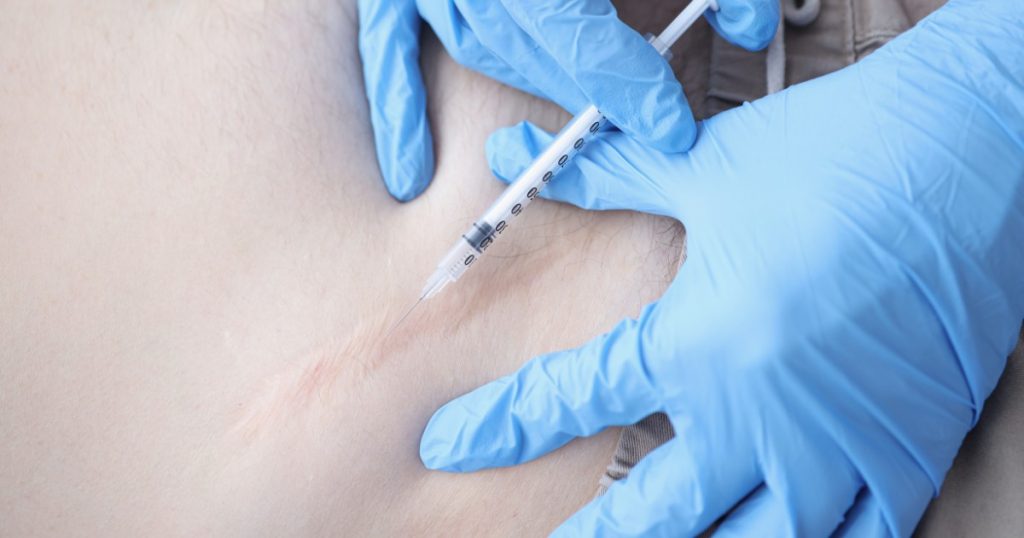
Intralesional steroid injections limit fibroblast proliferation and activity to slow or stop keloid growth.
- Inject excision sites at the time of closure
- Repeat injections every 4-6 weeks PRN
- Use high-concentration steroids for keloids
- Combine with 5-fluorouracil for some cases
- Preferred first-line treatment for growing keloids
- It can provide symptomatic relief as well
- Risk of atrophy telangiectasia with repeated use
Radiation prevents keloids from coming back.
Radiotherapy is commonly used as an adjuvant after keloid excision to limit recurrence.
- Interstitial brachytherapy is preferred for small scars
- Use fractionated external beam for larger keloids
- Still no consensus on optimal dosing protocols
- Tailor regimen based on a specific location
- Can combined with excision techniques
- Strictly shield radiosensitive tissues
- Lifelong monitoring required after radiation
Anti-inflammatory creams may prevent keloids.

Emerging topical options like imiquimod may limit keloid recurrence when used after procedures.
- Apply imiquimod nightly after excision
- Mechanism targets inflammatory mediators
- Studies show mixed results for prevention
- Seems most effective for small ear keloids
- Causes local irritation frequently
- Requires patient adherence to regimen
- The role is still being defined; more data is needed
Don’t scratch wounds if prone to keloids.
Excoriation and manipulation of healing wound beds can trigger pathologic inflammation.
- Causes minor but repeated trauma
- Damages fragile granulation tissue
- Interrupts extracellular matrix remodelling
- It can worsen pruritus, create a cycle
- This leads to abnormal collagen production
- Increases tension across scar
- Use silicone gel sheets to limit irritation
Wear sunscreen on healing scars.
Emerging data suggests sunlight can contribute to pathological inflammation during wound healing.
| Exposure | Impact | Strategy |
| UV radiation | Triggers inflammation | Use SPF 30+ sunscreen |
| Sunlight | Exacerbates responses | Reapply every 2 hrs |
| Laser therapy | Burns delicate skin | Consider wound covers |
Sun and other radiation can stimulate inflammatory pathways, interfering with routine healing. Cold Treatment for Scar Erasure is a method where cold is used to help reduce or remove scars. It’s like using ice to make a bruise feel better, but for scars. Keloid removal techniques include surgery laser treatments and steroid injections These methods help reduce or eliminate raised scars on the skin
Laser treatment prevents keloid scars.
Specific lasers can be used prophylactically after procedures to optimise the wound healing environment.
| Laser | Effect | Limitation |
| Pulsed-dye | Reduces TGF-beta | Minimal evidence |
| Fractional CO2 | Remodels matrix | Case reports only |
| Non-ablative | Limits fibrosis | Needs validation |
Early laser therapy may help optimise the healing environment, but more research is required.
Keloid scars can be disfiguring, painful reminders of trauma for prone patients. However, through evidence-based preventative strategies, new keloids do not have to be an inevitable outcome of surgery or injury. By combining gentle tissue handling, tension avoidance, anti-inflammatory drugs, radiation and occlusion techniques, practitioners can optimise the wound healing environment and avoid triggers known to veer heading down the path towards fibrosis. Patients also play a critical role in keloid prophylaxis through strict sun protection, avoidance of wound trauma, and adherence to physician recommendations like silicone gel sheets.
While research continues to refine treatment options for existing keloids, putting some of these basic preventative measures into practice today can help patients prone to overzealous healing hopefully achieve normal scarring instead. Addressing the question, “How do I prevent keloid scars?” individuals and surgeons alike can spare patients considerable psychosocial and physical burden for years.
Dr Shehzadi Tasneem Sultan, an esteemed plastic surgeon, specialises in body contouring and facial rejuvenation. With a medical degree and fellowship in plastic surgery, her extensive experience spans from the UK to Dubai. She offers a comprehensive range of aesthetic procedures, emphasising innovative techniques and patient-focused care.
Considering aesthetic enhancement? Book a consultation with Dr Shehzadi Tasneem Sultan for personalised and advanced plastic surgery solutions. Experience a transformation that uplifts your natural beauty and confidence. Book now to start your journey with a top-tier surgeon.












